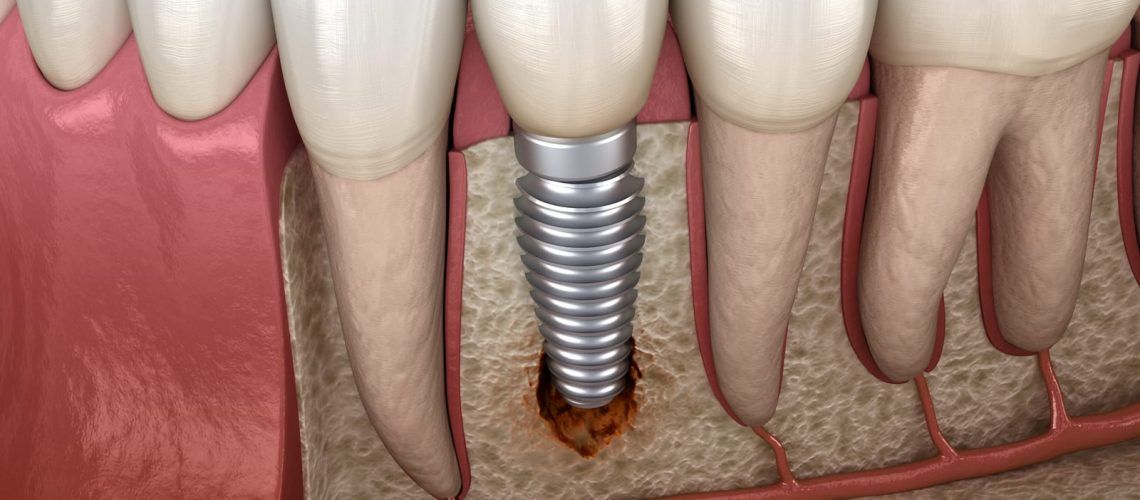
Dental implants have been increasing in popularity as they become more affordable and the technology and techniques involved become more refined. Like any normal medical procedure, there are potential complications that can arise during or after it is performed. Peri-implantitis is one form of complication that forms as the result of bacteria getting into the gums around the implant. This condition attacks the gums and the implant and can cause damage to both. Find out how to avoid developing peri-implantitis and how to identify it if you do.
Understanding The Causes of Peri-Implantitis And How To Identify It
Peri-implantitis shares many similarities with traditional gum disease, starting with how it develops. Periodontitis is caused by bacteria getting into the gums and beneath the gum lines resulting in the development of the gum disease known as gingivitis. When it goes untreated, it can develop into advanced gum disease or periodontitis. Peri-implantitis is also caused by bacteria that have formed in the gums and around the implant site. Common symptoms of this condition include:
- Swollen gums
- Tender gums
- Bleeding when brushing
- Oral sensitivity
You may recognize that these symptoms are similar to those caused by gum disease, and that’s to be expected. However, just as periodontitis can attack and damage the bones of the jaw, so can peri-implantitis. Worse, the infection caused by this condition is capable of damaging the implant itself, requiring it to be removed and replaced. If left untreated long enough, the bone can become damaged enough where the implant can no longer be supported and may fall out. Other symptoms to watch out for that can indicate peri-implantitis include:
- Pus discharge from inside the gums near the implant
- Lymph nodes located in the neck or armpits that are swollen
- Implant threads becoming exposed
- Gumline receding near the implant
- The implant feeling loose, like a loose tooth
- Soreness in the jaw can indicate bone loss
These indicate that the infection has advanced to a point where your implants, and indeed your overall health is in peril. It’s important if you notice symptoms like these that you speak to your oral health care provider to begin taking steps to address them.
How Peri-Implantitis Begins And What Can Be Done To Treat It
Peri-implantitis isn’t a common condition faced by dental patients, but it can occur in certain circumstances. The most common factors involved in the onset of peri-implantitis include the following:
- Immune System Compromised: Those patients who have implants and are affected by a disease or medical treatment that leads to their immune system being compromised are at greater risk of this condition. Diabetes, cancer treatment, and other systemic illnesses should be discussed with your dentist and medical professional when implants are present.
- Lacking Dental Care: Food particles and the bacteria that form as a result of them are common origin points for peri-implantitis. By maintaining proper dental care and seeing your dentist regularly, you can help avoid its onset.
- Parafunctional Habits: This term refers to behaviors that are involuntary, such as grinding your teeth, nail-biting, and how you position your jaw when it’s closed.
Treatment of the condition starts with regular dental care at home and seeing your dentist for your bi-annual checkups. In particularly severe cases, you may have to have the implant removed and a bone graft performed to restore the damaged bone. If you want to learn more, call and arrange a visit with your specialist today.